Improve Resident Well-Being. Strengthen Compliance. Equip Your Team — in 90 Days.
Our online ICE Dementia Care Framework gives staff a simple, repeatable process to manage behaviours without unnecessary medication — and keeps you inspection ready - year round
The Problem We Solve
Behavioural and Psychological Symptoms of Dementia (BPSD) — agitation, aggression, calling out — are among the toughest challenges in care.
Under pressure, Care homes may turn to antipsychotics, but regulations demand these are a last resort. With a clear, non-drug process in place, staff understand the behaviours they see, respond to underlying needs, resident well-being improves and inspection compliance strengthens.
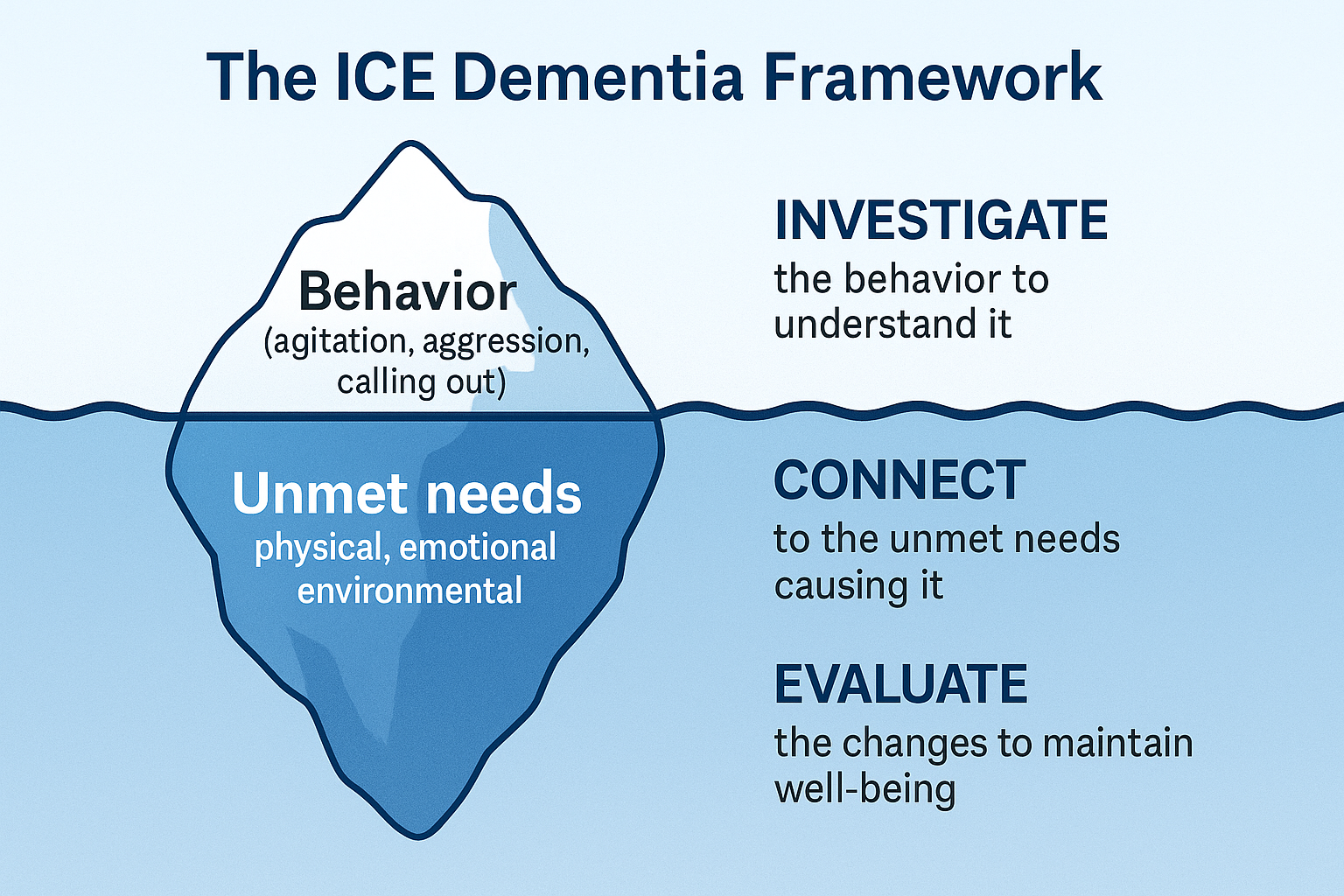
The ICE Dementia Framework
Investigate → Connect → Evaluate
Look beyond the behaviour - whats driving it?
- Investigate the behaviour to understand what's really happening
- Connect to the unmet needs (physical, emotional, or environmental) causing it
- Evaluate changes to maintain well-being over time
- This structured approach not only improves daily care, it also aligns with CMS and state requirements - leaving you with a clear, documented proof for inspections.
What All Regulators Expect
Even though inspection bodies differ from country to country, they all look for the same core principles in dementia care. At the heart of all of them is one idea:
staff must look beyond the behaviour to understand the unmet needs driving it.
1. Non-drug approaches first
Inspectors want to see that staff can pause, look beneath the surface, and identify what the behaviour is communicating — pain, fear, confusion, boredom, loneliness, hunger, overstimulation. Medication is never the starting point.
2. Regular and meaningful medication review
If an antipsychotic is used, there must be a clear reason, documented monitoring, and regular attempts to safely reduce or stop it. Staff must show that non-drug strategies have been tried and evaluated.
3. Safe, well-managed systems
Every PRN dose should be justified, reviewed, and clearly recorded. Behaviour monitoring, care-plan updates, and team communication must show a thoughtful, consistent approach.
4. Trained and confident staff
Regulators expect staff who understand dementia, recognise unmet needs, and respond calmly and compassionately — even during moments of distress.
5. Ongoing review and improvement
Care plans, team meetings, and daily notes should show continuous learning, reflection, and improvements in resident well-being.
How the ICE Approach Helps Staff Meet These Expectations
The ICE Dementia Framework teaches staff a simple, structured way to look beyond the behaviour and support the resident’s unmet needs:
- Investigate what the behaviour is communicating
- Connect it to the resident’s unmet needs
- Evaluate what changes, and adjust the plan
As staff learn to use ICE, their documentation naturally becomes clearer, more person-centred, and aligned with what all regulators want to see.
Your Evidence Binder then pulls everything together — making this learning and daily practice visible to inspectors.
For a detailed breakdown of how ICE aligns with regulations in the USA, UK, and Ireland, visit our Compliance Page.
Case Study: Paula
Before the ICE Dementia Framework
Paula refused personal care 5–6 times each week. This was distressing for Paula and highly stressful for staff. PRN medication was often used. However, this only managed the surface behaviour and did not address the underlying causes.
After 8 weeks using the ICE Dementia Framework
Refusals dropped to just 1–2 times per week. PRN use was reduced, and staff reported that personal care became calmer and more manageable.
Why it worked
Staff who knew Paula best were able to apply the ICE Dementia Framework, turning their daily knowledge into practical strategies.
Applying the ICE Dementia Framework
Investigate the behaviour of concern
Staff assessed Paula’s personal care experience from her perspective.
Connect to unmet needs
By reviewing the situation through Paula’s eyes, staff identified and addressed key factors, including:
-
The personal care environment
-
Paula’s experience of pain during care
-
Her understanding of what was happening and resulting anxiety
-
The way staff approached and communicated with her, ensuring consent
Evaluate changes to maintain well-being
Staff continued to monitor Paula’s needs daily, adapting strategies as circumstances changed.
The Result
A Paula-centred personal care approach that adapts to her needs, reduces distress, and promotes dignity and well-being.
Staff Reflections
“The course has helped me see the person, not just the dementia. I feel more confident in my care, and I can see the difference it makes in residents’ lives.”
Health Care Assistant
“The training gave me a deeper understanding of dementia — especially the importance of the environment and person-centred care. I now feel confident supporting families and sharing this approach with colleagues.”
Senior Nurse
“Since completing the training, I’ve slowed down to the residents’ pace, connected more personally, and rediscovered the enjoyment in my work.”
Care Staff Member
How It Works — 90-Day Path
Week 0–1: Pre-Training Audit & Manager Kickoff
Establish your baseline, set priorities, and align the team.
Weeks 1–8: Online Training & Application
Staff complete 10 modules. Each student selects one resident and develops a well-being plan as they progress through the course.
Weeks 8–12: Results & Next Steps
Review outcomes, compile your inspection-ready binder, and set the plan for the next quarter.
Fast-Track Option
For homes facing urgent inspection needs, significant progress can be achieved in just 30 days — with early results visible in staff practice and resident care.

